Health
The 4 Essential CPR Tools Every Medical Emergency Rescuer Should Have
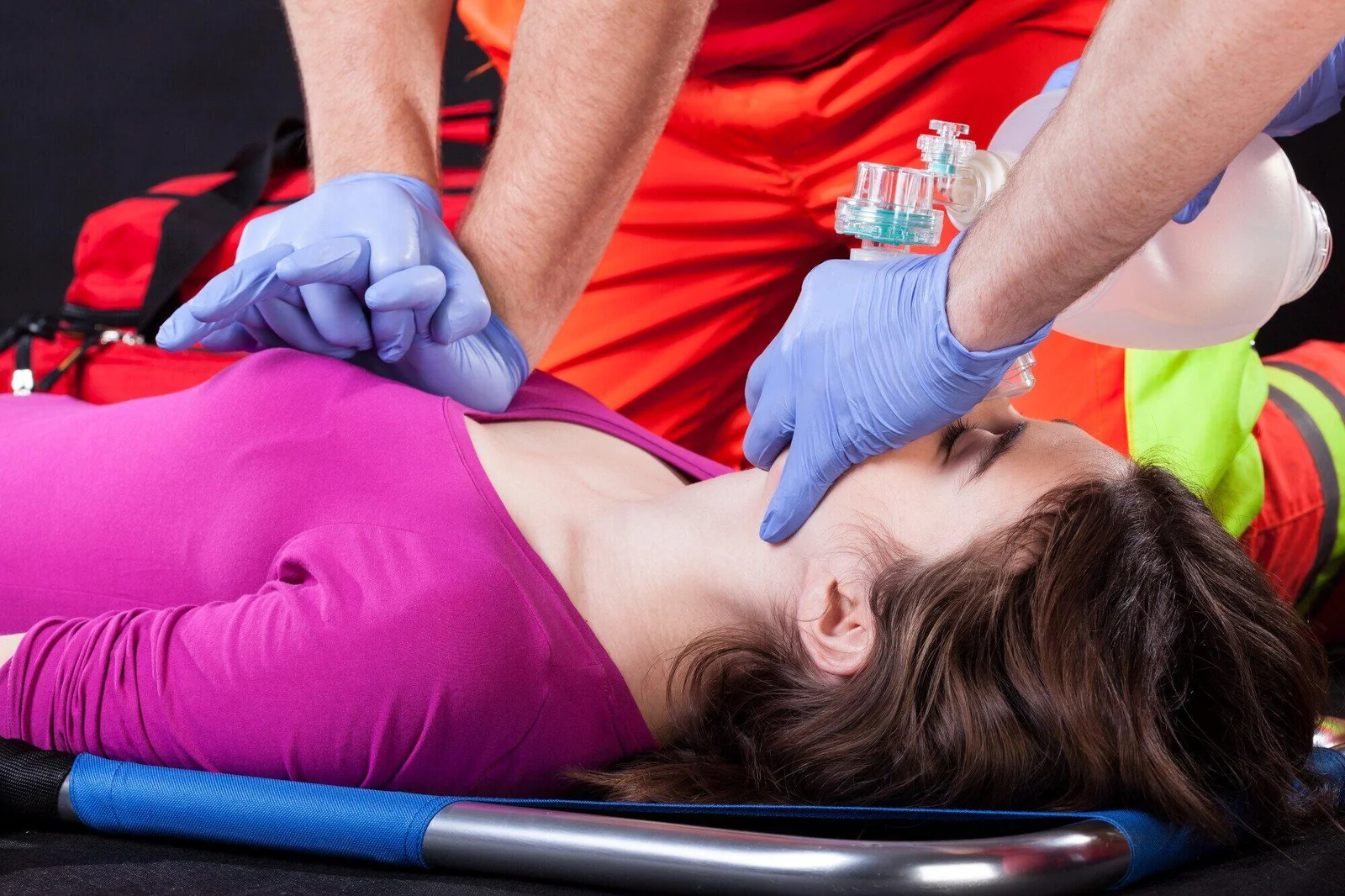
Are you ready to save a life? The importance of CPR (cardiopulmonary resuscitation) is crucial. In a medical emergency, having the right tools can significantly increase the chances of saving someone’s life. With so many options out there, it can be tough to know which tools you need.
Don’t worry! We’ve put together a list of the top must-have CPR tools for anyone ready to help in an emergency. Join us as we explore how each tool works and its benefits.
Let’s dive in and discover these tools every rescuer should have!
1. Pocket Mask or Barrier Device
Pocket masks or barrier devices are essential first aid supplies for anyone responding to medical emergencies. These devices create a protective barrier between the rescuer and the victim, helping to prevent the spread of infectious diseases. They also have a one-way valve, allowing rescuers to administer CPR safely and effectively.
For unconscious patients, pocket masks let you provide rescue breaths without direct mouth-to-mouth contact, making them a more hygienic choice. Lightweight and portable, these devices are easy to carry and can fit in a rescuer’s pocket for quick access during emergencies. They are a must-have for any medical professional and play a crucial role in saving lives.
2. Automated External Defibrillator
This small device is designed to deliver a shock to the heart during cardiac arrest, helping to restore a normal heart rhythm. It is a crucial tool because it significantly improves the chances of survival for individuals suffering from sudden cardiac arrest. AED devices are user-friendly and can be used by anyone, making them a valuable addition to any medical emergency team.
Besides, these devices are becoming more available in public places, making it easier to access and use them in time-sensitive situations. Ultimately, an auto defibrillator should be considered a crucial tool for any medical emergency rescuer to have at their disposal.
3. Face Shield
In a CPR situation, a face shield is vital in preventing the spread of diseases and ensuring the safety of the rescuer. It is compact and easily portable, making it convenient to carry at all times.
It also allows for proper ventilation during rescue efforts, ensuring that the victim receives enough oxygen. Every medical emergency rescuer should have a face shield as part of their standard equipment, as it can save lives and protect against potential health hazards.
4. Gloves
These thin, protective gloves provide a barrier between the rescuer and the patient’s bodily fluids, preventing the spread of infection and diseases. They are crucial in any medical emergency where there is a risk of coming into contact with blood, vomit, or other bodily fluids. In addition to protecting the rescuer, gloves also protect the patient by preventing any further contamination.
They are easy to use and can be quickly disposed of after use, making them a practical and necessary tool in any medical emergency responder’s kit. Without gloves, the risk of infection and transfer of diseases increases significantly, underlining the importance of having them as a standard tool in all CPR procedures.
Discover Essential CPR Tools Every Medical Emergency Rescuer Needs
Having the right CPR tools is crucial during a medical emergency. By equipping themselves with the essential CPR tool, medical emergency rescuers can ensure the best possible outcome for their patients. Don’t wait, make sure you have these tools on hand today to be prepared for any emergency.
Looking for more tips and advice? You’re in the right place! Make sure to bookmark our page and come back to check out more interesting articles.
Health
A Guide to Electronic Health Records: Everything You Need to Know

In the world of modern healthcare, Electronic Health Records (EHRs) have revolutionized the way patient information is managed. EHRs are digital versions of a patient’s paper chart, and they have become an integral part of the healthcare industry.
In this guide, we will delve into everything you need to know about Electronic Health Records. Read on.
What Are Electronic Health Records (EHRs)?
An Electronic Health Record (EHR) is a digital version of a patient’s medical history that is maintained over time by healthcare providers. Unlike paper records, EHRs are designed to be shared across different healthcare settings. This means that your health information can be accessed by various medical professionals, all in real time, such as:
- specialists
- pharmacists
- emergency room doctors
This helps to ensure better continuity of care. While EHRs are sometimes confused with Electronic Medical Records (EMRs), there is a distinction between the two.
How Do EHRs Work?
EHRs are built on software platforms that allow healthcare providers to input, store, and access patient data securely. They contain a wide range of information, including:
- Personal details
- Medical history
- Lab test results
- Medications
- Treatment plans
- Vitals
EHRs are typically cloud-based or stored on secure servers. It allows for easy access across various healthcare facilities.
Healthcare providers can access these records remotely. This improve collaboration and communication among specialists. One great example is the use of Behavioral Health EHR.
Key Features of EHRs
Patient Portal
Many EHR systems feature patient portals that allow patients to access their own medical records, schedule appointments, request prescriptions, and communicate with their healthcare providers online. This empowers patients to take an active role in managing their health.
Clinical Decision Support
EHRs can offer decision support tools that alert healthcare providers to potential issues, such as drug interactions or allergies, based on the patient’s medical history. This helps to improve patient safety and reduce errors.
Data Analytics
EHRs can analyze large sets of data to track trends, identify patterns, and provide insights into patient health. This is useful for population health management, improving clinical outcomes, and reducing healthcare costs.
Interoperability
EHRs are designed to be interoperable, meaning they can share information with other EHR systems and databases. This facilitates smoother transitions between healthcare providers, reduces redundancy, and ensures that no vital information is missed.
Security Features
Since EHRs contain sensitive health information, they come equipped with security features such as encryption, password protection, and multi-factor authentication. This helps ensure compliance with regulations like the Health Insurance Portability and Accountability Act (HIPAA) in the U.S., which mandates the protection of patient information.
Benefits of EHRs
Improved Care Coordination
One of the most significant advantages of EHRs is that they enable better coordination among healthcare providers. Whether a patient is:
- seeing a general practitioner
- seeing a specialist
- being admitted to the hospital
All providers can access the same up-to-date information. This helps avoid miscommunication, redundant testing, and ensures that all doctors involved are on the same page regarding the patient’s treatment plan.
Enhanced Patient Safety
EHRs help reduce medical errors by providing healthcare professionals with easy access to comprehensive patient data. Alerts for drug allergies, potential drug interactions, and abnormal lab results can be automatically triggered. This prevents dangerous mistakes that might otherwise occur with paper records.
Streamlined Workflow
By digitizing patient records, EHRs eliminate the need for physical paperwork, reducing time spent on filing, retrieving, and updating records. This leads to improved workflow efficiencies in healthcare settings. It allows doctors and nurses to spend more time with patients rather than paperwork.
Better Patient Engagement
With features like patient portals, EHRs enable patients to access their medical records, track their health data, and communicate directly with healthcare providers. This can help increase:
- patient engagement
- adherence to treatment plans
- overall satisfaction with their care
Cost Savings
EHRs can reduce the overall cost of healthcare by:
- improving efficiency
- reducing redundant tests,
- preventing medical errors
When healthcare providers share accurate, real-time information, it reduces the need for repeated diagnostic procedures and minimizes the chances of treatment delays.
Research and Public Health Benefits
EHRs also play a key role in research and public health initiatives. Data from large populations can be anonymized and used for studies to:
- identify trends
- improve treatments
- develop new medical insights
Challenges of EHRs
Implementation Costs
One of the main challenges with EHR adoption is the upfront cost. While the long-term savings can be substantial, the initial expense of purchasing EHR software, training staff, and integrating the system into an existing practice can be prohibitive for some healthcare providers. Especially smaller clinics and rural practices.
Technical Issues
EHR systems can sometimes suffer from technical problems, such as:
- software glitches
- system downtimes
- issues with interoperability
These technical hurdles can disrupt healthcare services and create frustration for both providers and patients.
Data Security Concerns
While EHR systems are designed with strong security features, they are still vulnerable to cyberattacks and data breaches. High-profile incidents of healthcare data breaches have raised concerns about the privacy and security of sensitive patient information.
Training and Usability
Effective use of EHR systems requires proper training for healthcare providers. The learning curve associated with new technology can be steep. Also, poorly designed interfaces may result in decreased efficiency and increased errors.
Patient Privacy
Despite encryption and security measures, the digital nature of EHRs raises concerns about patient privacy. The more widespread the use of EHRs, the greater the potential for unauthorized access to personal health data. This is either through hacking or human error.
The Future of EHRs
As technology continues to advance, so too will the capabilities of Electronic Health Records. The future may bring even greater interoperability. This makes it easier for patients to share their medical records across different healthcare systems worldwide.
Artificial intelligence (AI) could also play a role in improving EHR functionality. It help doctors make faster, more accurate diagnoses and treatment decisions based on data-driven insights. In addition, the rise of telemedicine and remote patient monitoring could further enhance the role of EHRs in providing comprehensive, real-time care.
Use Electronic Health Records Now
In conclusion, electronic health records have transformed the healthcare industry and have become an essential tool for healthcare providers worldwide. Understanding the benefits and functionalities of EHRs is crucial for the future of healthcare delivery.
Start utilizing EHRs today and witness the positive impact it can have on your practice! Don’t wait, join the digital revolution and see the difference it can make. Get started now!
If you want to read more articles, visit our blog.
Health
The Surge of Addiction in America’s Top Professions: Understanding the Growing Crisis

Key Takeaways
- Addiction is rising in high-stress fields, including healthcare, law, finance, and emergency services.
- Stress, long hours, and pressure contribute to increased substance abuse in these demanding professions.
- Seeking support through treatment, company wellness programs, and lifestyle changes can make a significant impact.
Introduction
Across the United States, addiction has become a hidden crisis in many of the most respected professions. Many professionals deal with overwhelming stress and intense demands in healthcare, law, finance, and emergency response. These high-stakes roles can sometimes drive people toward substance abuse as a way to cope with the pressure.
In this article, we’ll explore why addiction rates are rising in specific fields, how this affects personal and professional lives, and what steps professionals and workplaces can take to find support. Acknowledging this issue and finding help can lead to healthier, more balanced lives.
Why Certain Professions Face Higher Risks of Addiction
Specific work environments place people at a higher risk for addiction. The combination of stress, limited downtime, and sometimes even access to substances can make it difficult for individuals to manage their well-being effectively.
Workplace Stress and High Expectations
High-stakes environments often mean high expectations. Whether it’s doctors making life-or-death decisions, lawyers working on complex cases, or financial professionals managing significant investments, the pressure can feel unending. For many, alcohol or other substances become a way to unwind or escape after a tough day.
Extended Hours and Lack of Work-Life Balance
Many professionals work long hours, sacrificing personal time and self-care. This lack of balance can make it hard to develop healthy coping mechanisms. Extended work hours mean less time with family, limited social life, and even fewer opportunities to relax, leaving individuals vulnerable to stress and, ultimately, addiction.
Access to Substances
In some fields, especially healthcare, substances are more accessible. For example, Doctors, nurses, and pharmacists may have easy access to certain medications, which can increase the risk of misuse. When combined with high stress, this access creates a dangerous scenario where professionals might start using substances they encounter daily.
Professions Most Affected by Addiction in America
Addiction is not limited to any one profession, but some fields face higher risks. Let’s examine these professions and the unique challenges each one faces.
Healthcare Professionals
Doctors, nurses, and other healthcare providers face significant stress, long hours, and, often, emotional burnout. They work in high-pressure situations, handling life-and-death cases while caring for patients. With more accessible access to medications, some healthcare workers turn to substances for relief, making healthcare one of the most affected fields for addiction.
Legal Professionals
Lawyers and judges often work in highly competitive and demanding environments. Long hours, intense workloads, and high expectations can lead to substance use as a way to handle stress. Alcohol is a common coping mechanism in the legal field, with some legal professionals turning to it after long days in the office or courtroom.
Finance and Corporate Professionals
Success often depends on performance in finance and corporate environments, which can lead to intense pressure. Many professionals in this field work long hours under high stress, especially when dealing with market fluctuations or essential deals. This pressure can drive some to use substances to unwind or stay alert during long work hours.
First Responders
Police officers, firefighters, and paramedics often experience high-stress situations and exposure to traumatic events. The demands of their jobs and the trauma they witness can lead to alcohol or substance use as a way to cope. Addiction in this field is often tied to the need to manage both physical and emotional pain, making it an area of concern for those working to keep others safe.
The Impact of Addiction on Personal and Professional Life
Addiction affects not only the individual but also their job performance, relationships, and health. In high-stress professions, these impacts can be particularly significant.
Health and Mental Well-being
Addiction often leads to physical and mental health issues, including anxiety, depression, and exhaustion. Substance abuse can weaken the immune system, disrupt sleep patterns, and lead to serious long-term health problems. The toll on health makes it challenging to maintain the energy and focus needed for demanding jobs, leading to a cycle of addiction and decreased well-being.
Job Performance and Relationships
Addiction affects job performance, causing missed deadlines, reduced productivity, and poor decision-making. These impacts can strain relationships with coworkers and superiors. Over time, addiction can lead to disciplinary action or even job loss, creating further stress for the individual.
The Cycle of Addiction in Work Environments
Some workplace cultures unintentionally encourage substance use as a means of stress relief, mainly when social gatherings or work events include alcohol. This creates a cycle where addiction is normalized, making it harder for individuals to recognize they need help. It’s essential to foster awareness and healthy coping mechanisms in these environments to break the cycle.
How to Seek Help and Find Support in the Workplace
If you or a colleague is struggling with addiction, know that help is available. Here are some steps to find support and create a healthier work environment.
Recognizing Signs of Addiction
The first step to finding help is recognizing signs of addiction, such as increased use of substances, difficulty concentrating, or mood changes. Awareness of these signs, whether in yourself or a coworker, is essential for taking action.
Resources and Treatment Options
Many companies offer resources such as Employee Assistance Programs (EAPs), which provide counseling and referrals for addiction treatment. Other options include therapy, addiction treatment centers, and support groups. Seeking out these resources can make a significant difference and provide the support needed to manage addiction.
Creating a Healthier Work Environment
Employers can play an essential role in supporting employees by promoting a healthier workplace. Programs that focus on wellness offer flexible schedules and provide resources for stress management, which can help reduce the pressure that leads to substance use. Workplaces encouraging open conversations and prioritizing mental health create a culture where people feel comfortable seeking help.
Conclusion
The rise of addiction in America’s top professions highlights the need for greater support and awareness in high-stress careers. Acknowledging this issue is the first step toward finding solutions. By understanding the causes, seeking help, and creating supportive work environments, professionals in healthcare, law, finance, and emergency response can take steps toward healthier lives.
If you or a loved one is facing addiction in a challenging profession, contact Virtue Recovery Center at 725-777-5685. Our team offers compassionate, confidential support to help you take the first steps toward recovery.
FAQs
Why are some professions more prone to addiction?
High-stress environments, long hours, and easy access to substances make some professions more vulnerable to addiction.
What professions have the highest addiction rates?
Healthcare, law, finance, and first responders have some of the highest addiction rates due to intense stress and responsibilities.
How does addiction affect job performance?
Addiction can lead to poor productivity, impaired decision-making, and strained relationships with colleagues, affecting job performance.
What are the first steps for professionals seeking help?
Recognizing the problem and contacting a trusted resource, such as an EAP or treatment center, are good first steps toward recovery.
Health
Navigating Clinical Trials: A Patient’s Perspective

What Are Clinical Trials?
Clinical trials are structured research studies where scientists and doctors delve into the safety and efficacy of medical strategies and innovative treatments involving human volunteers. They bridge scientific research and formally introduce new medicines and techniques for public use. From preventative trials to lower the chance of acquiring illnesses to treatment studies that assess novel medications, surgical techniques, or behavioral tactics, different sorts of trials serve distinct stages and requirements of research. Each trial can be distinctly categorized into phases. In Phase I, the primary focus is safe dosage range determination and initial safety, while Phase II dives deeper into effectiveness and potential side effects. Phase III involves rigorous comparison with standard treatments, concluding with Phase IV, which tracks long-term effectiveness post-approval. These trials often encompass numerous participants over extended periods and offer unique insights into groundbreaking medical advancements.
Clinical trials for breast cancer play a pivotal role by offering opportunities to experience and contribute to innovations in healthcare. Volunteers can gain early access to new treatments and contribute significantly to understanding and developing therapies that could benefit future generations.
Benefits of Participating in Clinical Trials
There are several possible benefits to taking part in clinical trials. On a personal level, becoming a trial participant offers the chance to access cutting-edge therapies that are not yet available to the public. It can benefit those with diseases for whom there are few available treatments or those who have not responded well to current medicines. Beyond personal health benefits, the broader impact cannot be overstated — participants in clinical trials contribute to a worldwide pool of knowledge that drives medical progress. This collective input of data helps scientists and doctors understand diseases better, ultimately leading to the development of more effective treatment options.
Historically, numerous life-saving treatments we now consider standard were born from clinical trials. For instance, developing vital vaccines and advanced therapies for conditions like cancer and heart disease have relied heavily on carefully conducted clinical studies. These trials remain a cornerstone of medical advancement, continually shaping the healthcare landscape for years.
Understanding Patient Rights and Informed Consent
Entering a clinical trial requires a solid understanding of your rights and the informed consent process. This fundamental step, illuminated by resources from institutions like the National Institutes of Health, ensures that participants are fully aware of the trial’s scope, the methodologies used, and any foreseeable risks or benefits. Informed consent is a formality and a crucial conversation between the potential participant and the research team. It respects the individual’s autonomy, enabling a well-informed decision about participation.
Fundamental rights include:
- The right to receive comprehensive information about the trial before deciding to participate.
- The right to ask questions and have them answered satisfactorily.
- The freedom to withdraw from the trial at any point without affecting your future medical care.
Understanding these rights can empower participants to make better-informed decisions, ultimately enhancing their overall experience in the trial.
How to Find Suitable Clinical Trials
Finding a suitable clinical trial starts with conducting thorough research. With numerous trials happening simultaneously worldwide, identifying one that aligns with your condition and health goals is crucial. Online databases and registries fall into this category; they serve as vital resources by cataloging detailed information about ongoing clinical trials. Participants can filter entries based on condition, location, or trial phase criteria.
Moreover, discussions with healthcare providers can provide a wealth of information; professionals can offer insights into trials that might not be immediately apparent through research alone and help you assess eligibility criteria and potential outcomes. Open communication with your healthcare teams ensures your steps align with your broader health management strategy.
Factors to Consider Before Enrolling
Choosing to participate in a clinical study is a serious decision. Participants must comprehensively evaluate several critical factors, including protocols, eligibility requirements, and logistical considerations like duration and location. Defining potential risks versus benefits forms a vital part of this evaluation.
Furthermore, involving your primary care physician in this decision-making process can provide additional insights and reassurances. They can ensure the trial aligns with your broader health objectives, minimizing potential conflicts with existing treatments or health conditions.
Clinical Trials’ Contribution to Medical Advancement
Clinical trials feature prominently in the tapestry of medical history. They have led to the discovery of innovative treatments and pioneered methods that reshape preventative measures, diagnostic tools, and therapeutic strategies worldwide. For example, controlled trials significantly advanced the development of penicillin and insulin, two cornerstones of modern medicine.
Significant trends have further underscored their importance in recent years. As we look to the future, trials offer an avenue for incorporating precision medicine and personalized treatment strategies, a concept currently gaining momentum. Staying informed with platforms like Science.org can illuminate the most recent advancements driven by clinical trial outcomes.
Common Misconceptions About Clinical Trials
Misconceptions about clinical trials can sometimes deter individuals from participating. One common myth is the belief that trials are unsafe or exist merely to test unproven treatments without care for participant well-being. In reality, trials adhere to strict regulatory standards designed to safeguard participants. Frequent layers of oversight from governmental and independent ethical bodies strive to guarantee safety and integrity.
The concern regarding placebos and receiving “no treatment” also prevails. While placebos are used, they are primarily in comparative studies where withholding active treatment would not result in harm. Often, trials compare the new treatment against a current standard to assess comparative efficacy.
Tips for Maximizing Your Experience in a Clinical Trial
To optimize your clinical trial experience, consider fostering effective communication with trial coordinators. They can provide invaluable support and clarification, ensuring your journey through the trial is as seamless as possible. Maintaining a personal health journal can also offer dual benefits: tracking progress and any changes you feel and providing data to healthcare providers.
Support groups can serve as excellent adjunct resources, offering peer support, shared experiences, and insights that help build resilience and provide emotional comfort. Whether online or in person, they can connect you with others who understand the unique experiences inherent to trial participation.

 Entertainment6 months ago
Entertainment6 months agoSandra Orlow: Exploring the Life and Legacy of a Cultural Icon

 Business7 months ago
Business7 months agoTex9.Net Crypto: Fast, Secure International Money Transfers with Competitive Rates

 General2 months ago
General2 months agoBaby Alien Fan Bus: Watch Parts 2 & 3 on Twitter, Reddit!

 General2 months ago
General2 months agoDiana Nyad & Bart Springtime: A Swim to Success

 Business7 months ago
Business7 months agoSnapchat Planets: Exploring Your Streak Universe

 General5 months ago
General5 months agoDeeper Dive into myfavouriteplaces. org:// blog

 Business7 months ago
Business7 months agoWhat is O Farming: How to Make Money Online and Its Start-Up Benefits

 Business7 months ago
Business7 months agoFintechZoom Apple Stock: Real-Time Insights and Expert Analysis